How Our Medical Office Can Help With Your Rheumatoid Arthritis (RA)
“Rheumatoid arthritis differs from osteoarthritis in that it not only causes joint pain and stiffness, but can also affect other body systems. RA often affects younger adults, which can impair ability to work. If you have joint pain and stiffness, regardless of your age, you should come in and see us- there are treatments that can help”.
What is rheumatoid arthritis?
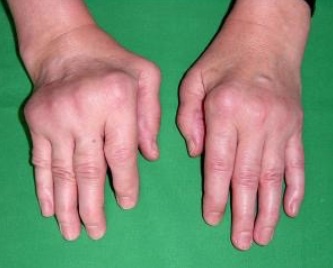
 Rheumatoid arthritis (RA) is an autoimmune disorder in which the body attacks itself- usually the small joints of the hands and feet, although any joint may be affected by RA. It is the most common type of autoimmune arthritis. Women are affected more often than men (3:1). It is estimated that over 1 million people in the US are living with RA, many of them relatively young. Rheumatoid arthritis most often affects people in their 40s, 50s and 60s, but it can occur at any age (when the disease is diagnosed in children it is called juvenile arthritis)
Rheumatoid arthritis (RA) is an autoimmune disorder in which the body attacks itself- usually the small joints of the hands and feet, although any joint may be affected by RA. It is the most common type of autoimmune arthritis. Women are affected more often than men (3:1). It is estimated that over 1 million people in the US are living with RA, many of them relatively young. Rheumatoid arthritis most often affects people in their 40s, 50s and 60s, but it can occur at any age (when the disease is diagnosed in children it is called juvenile arthritis)
What are the symptoms of rheumatoid arthritis?
The joint pain of RA is often at its worst in the morning when you first wake up. You may find it difficult to move the affected joints well and without pain when you first wake up. The pain may improve as the day wears on; as the disease progresses, or during acute flares of the disease, pain may be constant.
Because RA is an autoimmune disease, other organs of the body may be affected as well. You may also experience:
- loss of appetite
- fever
- fatigue
- dry eyes and mouth
- rheumatoid nodules (firm mobile lumps that grow under the skin in the hands, elbows)
- lung problems
- anemia (low number of red blood cells)
What causes rheumatoid arthritis?
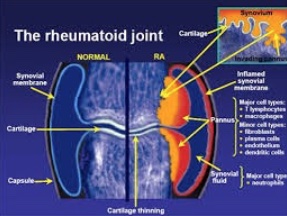
 While experts understand that RA is an autoimmune disease, no one knows what triggers the immune system to attack the synovial membrane of a joint. The synovial membrane is the tissue that lines the joint. The immune system releases chemicals that attack this lining, as well as the cartilage that cushions the joints and the joints themselves. It is likely that some people are genetically susceptible and the disease is triggered by an unknown event.
While experts understand that RA is an autoimmune disease, no one knows what triggers the immune system to attack the synovial membrane of a joint. The synovial membrane is the tissue that lines the joint. The immune system releases chemicals that attack this lining, as well as the cartilage that cushions the joints and the joints themselves. It is likely that some people are genetically susceptible and the disease is triggered by an unknown event.
What can I expect when I come for my visit?
If you suspect that you may have RA, it is best to come see us as soon as possible. Early treatment can help prevent disease progression, and RA requires constant monitoring to prevent destruction of joints.
We will start off by taking a history from you. We’ll need to know about your past medical history, medications you are currently taking and any allergies you may have. We will then ask you to tell us about your symptoms: when did they start, when is the pain at its worst and what makes the pain better or worse. We may also ask whether you have noticed any fever, excessive tiredness or other constitutional symptoms.
Once we have learned more about your symptoms, we will want to examine your joints, particularly the joints of your wrists, hands and feet. We will look at your other joints as well. We will be looking for redness, swelling and warmth, as well as pain with manipulation of the joints.
Unfortunately, there is no single test we can order that can tell us whether or not you have arthritis, but there are blood tests that can provide clues. If we suspect you may have RA, we might order numerous blood tests that may provide supporting evidence to the diagnosis. These blood tests might include:
- complete blood count- to check for anemia
- rheumatoid factor- a protein found in the blood of many people with RA (although not all)
- erythrocyte sedimentation rate- a non-specific marker for inflammation which can be elevated in many conditions including RA
- anti-CPP- blood test to look for antibodies to certain peptides found in the blood of some people with RA
Although x-rays may not be helpful in the early stages of RA, they can be used to mark the progress of the disease. X-rays in the first months of RA may appear normal, but that does not mean you don’t have RA.
Can Advanced Cardiology & Primary Care LLC Treat my Symptoms?
We are internal medicine physicians with a specialty in geriatric medicine. We can help you manage your disease. If necessary, we would refer you to a rheumatologist to confirm your diagnosis and make treatment recommendations. Many people see a rheumatologist periodically and depend on their primary care doctor to manage their condition the rest of the time. It can be difficult to get in to see a specialist when needed- for this reason, you will need a physician you can depend on to treat you between visits to a specialist. We would love to partner with your rheumatologist to help you with your condition.
Today, there are many treatment options for RA. Medications can help you live a relatively healthy and normal life and can induce remissions in the active disease process. If you think that you may have RA, it is important that you receive a proper diagnosis and begin treatment to prevent worsening of the disease. Make your appointment today.
